What the 2027 Changes to Radiology Reporting Mean for Imaging Leaders
Written by
Chuck Nagel
Healthcare Business Partner
Last Updated: April 9, 2026
Upcoming 2027 reporting changes from the Joint Commission and National Quality Forum (NQF) will fundamentally reshape how radiology departments track, interpret, and act on patient safety events, making accurate, timely radiation data more critical than ever.
Having spent much of my career leading imaging departments and serving as a Radiation Safety Officer, I’ve learned that regulatory changes rarely stay confined to policy updates. They ultimately shape workflows, influence decision-making, and affect how teams can document and defend their processes.
The upcoming 2027 changes to radiology reporting will be one of those moments that directly impacts how imaging teams operate day to day.
Key Takeaways
- Radiology reporting will shift to a standardized 28-event SRE framework by 2027 while maintaining the existing TJC sentinel event standards
- Imaging-related risks (including radiotherapy errors and missed results) are directly impacted
- Events will be evaluated based on whether they are serious and largely preventable
- Standardization will reduce ambiguity and increase accountability
- Strong data, including dosimetry, will be essential for compliance and decision support
Understanding the 2027 Shift in Radiology Reporting
Many radiology leaders are beginning to hear about the Joint Commission’s upcoming alignment with the National Quality Forum (NQF). At first glance, it may seem like another reporting update. In reality, it represents a broader shift.
Over the course of nearly two decades in hospital imaging leadership – including roles as Director of Imaging Services, Emergency Management Chair, and Radiation Safety Officer (RSO) – I’ve seen how regulatory changes move from guidance to expectation, and eventually into day-to-day operations. Whether it was overseeing interventional radiology, CT, MRI, nuclear medicine, or supporting system-wide safety initiatives, the common thread was always the same: what starts as policy quickly becomes operational reality.

On January 1, 2027, the Joint Commission will align its Sentinel Event framework with the updated list of 28 Serious Reportable Events (SREs) from the NQF. This change introduces a more standardized approach to defining and evaluating patient safety events – one that will directly impact radiology departments.
My experience reinforced something important: when standards become more aligned across organizations, expectations become clearer, more consistent, and more closely scrutinized.
From my perspective, this shift is about clarity. It’s about understanding what occurred, why it occurred, and whether your team can support those conclusions with confidence – not just internally, but in a way that stands up to external review.
In radiology, where workflows are complex and responsibilities often span multiple departments, that level of clarity doesn’t happen by accident. It requires intentional processes, reliable data, and a clear understanding of where risks actually exist.
What’s Changing and Why It Matters
Radiology safety/near miss reporting has often been somewhat subjective and historically shaped by multiple frameworks – each with its own unique categories, often requiring an event to fit into a predefined box. That has often led to inconsistent reporting and inaccurate data.
I’ve worked within those environments, and I suspect many imaging leaders have as well.
The 2027 update is intended to address the areas largely considered the greatest opportunity and the greatest risk for preventable harm by aligning these reporting opportunities under a single, standardized structure.
The updated SRE framework defines 28 events, applies across all care settings (including outpatient imaging), and introduces clearer criteria for what qualifies as a reportable event.
The 28 SREs are organized into four categories:
- Procedural Events
- Product or Device Events
- Patient Protection Events
- Care Provision Events
Of the 28 events, 13 are already recognized under the current Sentinel Event framework, while 15 will be newly formalized – introducing additional reporting expectations that many imaging teams are not currently structured to capture.
While this alignment simplifies the structure, it also raises expectations. As definitions become more consistent, so does the level of accountability.

It’s also important to recognize that more than 30 states and many healthcare systems already use versions of the NQF SRE framework for required or voluntary reporting. As federal and accreditation standards align, organizations operating across multiple states may begin to see greater consistency in reporting expectations – but also less flexibility in interpretation.
For many organizations, this will shift reporting from a largely interpretive process to a more criteria-driven one. Events will increasingly be evaluated against clearly defined thresholds – particularly whether they are tied to a patient encounter, resulting in harm, and were considered preventable under current standards of care.
The shift reduces subjectivity and also increases the need for documentation, consistency, and supporting data.
For a deeper breakdown of how structured programs support compliance, see our Complete Dosimetry Program Management Guide: Setup, Compliance & Cost Optimization.
Where Radiology Is Directly Impacted
Although the SRE framework spans the broader healthcare system, several events have direct relevance to imaging and radiology operations.
These include radiotherapy delivery errors, MRI-related safety events, and failure to act on radiology results – an area that often presents both clinical and operational challenges.

It is also important to understand how these events are classified. Some must be reported regardless of outcome, while others require evidence of serious patient harm that was largely preventable.
That distinction is more than technical: it influences how teams document events, how they escalate concerns, and how they ultimately explain their decisions.
In practical terms, imaging teams should expect closer scrutiny around:
- MRI safety controls, including Zone IV access and device and other ferrous object screenings
- Radiotherapy delivery accuracy and dose thresholds
- Communication and follow-up on critical radiology findings
- Equipment- or workflow-related events that could lead to patient harm
For a foundational overview of monitoring technologies that support these decisions, explore the Guide to Radiation Dosimeter Types: TLD, OSL & Digital Technology Comparison.
Operational Pressure Points to Anticipate
From an operational standpoint, changes like this tend to surface existing challenges rather than create new ones.

One area that will require attention is interpretation. Even with clearer definitions, teams must still determine whether an event meets reporting criteria. Questions around severity and preventability are not always straightforward, particularly when decisions must be made quickly.
Another consideration is coordination. Many radiology-related events involve multiple departments. A failure to act on a radiology result, for example, often reflects a breakdown in communication or workflow rather than a single point of failure.
Perhaps most importantly, there is the need to confidently support decisions after the fact.
It is one thing to manage an event internally; it is another to clearly explain what occurred, why it occurred, and how it will be prevented moving forward.
In many cases, these challenges are not new – they’ve simply been tolerated within less standardized frameworks. What changes in 2027 is not the existence of these issues, but the expectation that they are consistently identified, classified, and addressed.
Learn what hospitals should be asking about their dosimetry service in our Q&A video with industry thought leaders, RDC President Chris Passmore, CHP, and Senior Vice President of Operations & Technical Services Mirela Kirr: Radiation Safety Q&A.
The Growing Role of Data in Radiology Reporting
As reporting becomes more standardized, data becomes more central to the process. This is where dosimetry plays a meaningful, though often understated, role.
This is where many radiology programs will feel a gap. It’s not uncommon for dose data to exist, but not in a form that is easily accessible, actionable, or connected to event evaluation workflows. When data is delayed, fragmented, or difficult to interpret, it limits a team’s ability to confidently assess whether an event represents normal variation or a true deviation.
Accurate dosimetry data provides objective context and allows teams to determine whether exposures were consistent with expectations or whether something deviated from normal patterns.
With a lower limit of detection (LLD) of 1 mrem across OSL and TLD passive dosimeter badges and NetDose™ digital dosimeter, Radiation Detection Company’s whole body radiation monitoring solutions provide the data resolution needed to distinguish true exposure deviations from normal variation – supporting more confident event evaluation, not just after an incident, but before patterns escalate into reportable events.
Explore all whole body dosimetry solutions →
When paired with AI platforms like MyRadCare Insights™, digital dosimeters can support earlier identification of trends. Most serious events develop over time, often through small deviations that may go unnoticed without consistent monitoring.

Without accurate data, assessments can quickly become subjective. That distinction becomes especially important under a framework that evaluates events based on whether harm occurred and whether it was preventable.
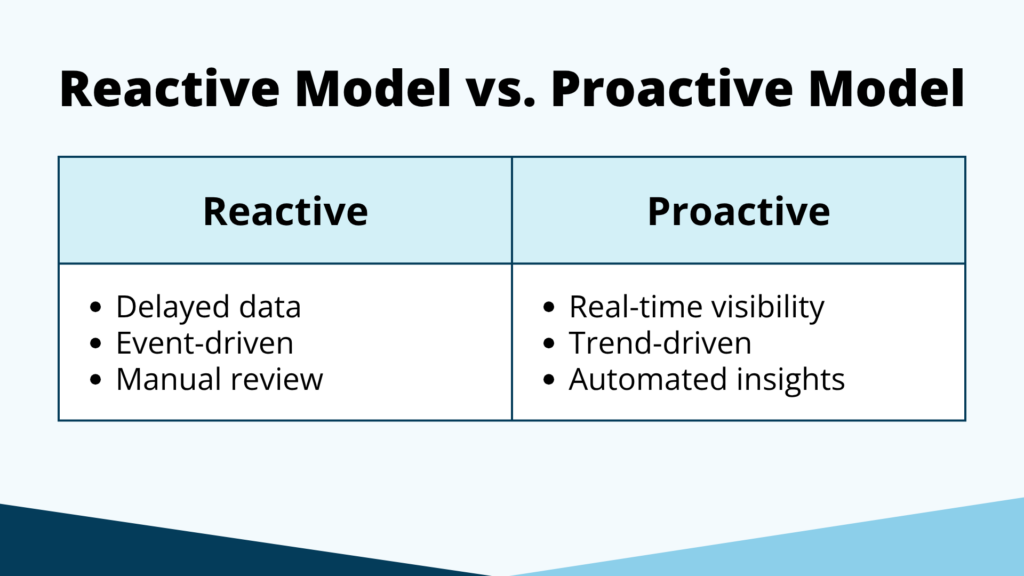
As reporting expectations increase, the ability to move from retrospective review to proactive monitoring becomes more important. Organizations that can identify trends earlier (before they meet reporting thresholds) will be in a much stronger position both operationally and from a compliance standpoint.
For a broader view of how digital dosimeters like NetDose™ can support proactive radiation monitoring, see Digital Dosimetry and AI: Shifting from Reactive to Proactive Radiation Safety.
A Shift Toward Standardization and Visibility
At a broader level, these changes reflect a continued movement toward greater standardization and transparency in healthcare.
The intent is to reduce variability, improve consistency, and ultimately enhance patient safety outcomes. These are positive developments for the industry.
At the same time, increased visibility means that processes, decisions, and data will be examined more closely. Organizations that rely on informal practices or fragmented information may find that more challenging.
Radiology reporting isn’t the only area undergoing change. See How DBT, CEM, & Emerging Technologies Are Reshaping Mammography Radiation Safety.
How I Would Approach This Today
If I were currently leading an imaging department or serving as an RSO, I would approach this less as a regulatory change and more as an operational readiness exercise.
I would focus on three practical areas:
- Reviewing current reporting workflows to identify ambiguity
- Ensuring data is accessible, timely, and actionable
- Shifting focus from isolated incidents to trend identification

For teams looking to strengthen compliance readiness, resources like the Radiation Compliance Cheat Sheet and Digital Dosimetry Checklist can provide a helpful starting point.
For organizations currently evaluating their dosimetry provider ahead of the 2027 deadline, our SwitchAssist™ onboarding process makes it possible to transition without disrupting an active compliance program.
If you're evaluating how your current dosimetry program supports reporting, compliance, and operational efficiency, it's worth having a conversation with a team that understands both the clinical and regulatory side of radiation safety.
Call 800.250.3314 or contact Radiation Detection Company to speak with a radiation safety expert ahead of the changes.
Preparing for What’s Ahead
Changes of this nature rarely arrive all at once. They tend to emerge gradually through audits, internal reviews, and evolving expectations.
Over time, those incremental changes reshape how organizations operate.
The teams that adapt most effectively will not be those reacting to the requirements in 2027, but those who have already strengthened their processes, improved their data visibility, and developed a clearer understanding of their risks.
From my perspective, that preparation is where the real opportunity lies.
Get Expert Support for Your Radiation Safety Program
If you’re evaluating how your current dosimetry program supports reporting, compliance, and operational efficiency, our team is here to help.
Call 800.250.3314 to speak with a radiation safety expert →
Complete our contact form to connect with our dosimetry team →
Frequently Asked Questions
What is changing in radiology reporting in 2027?
The Joint Commission will align its Sentinel Event framework with the NQF Serious Reportable Events list, standardizing how patient safety events are defined and reported.
Do these changes apply to outpatient imaging centers?
Yes. The updated framework applies across all care settings, including outpatient and ambulatory imaging environments.
Will this increase reporting requirements?
While it may not increase the number of events, it will improve clarity and consistency, which may lead to more events being formally recognized.
Why is this important for radiology teams?
Several of the defined events directly involve imaging workflows, including radiotherapy, MRI safety, fluoroscopic effects, and communication of results. The upcoming 2027 changes to radiology reporting will be one of those moments that directly impacts how imaging teams operate day to day – especially in how preventable events are classified, investigated, and ultimately reduced or eliminated.