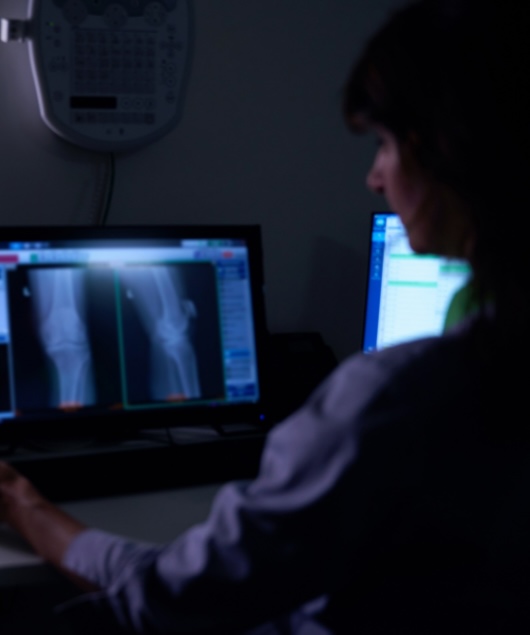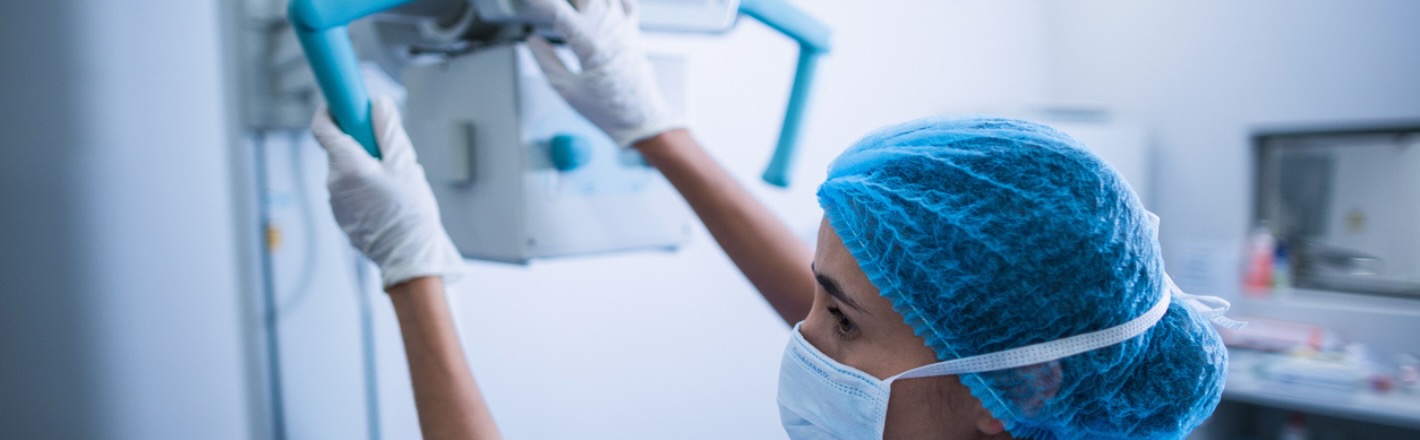
Radiation Risk in Healthcare Imaging: The Hidden Tradeoff Between Comfort and Protection
Reviewed by
Chris Passmore, CHP
President, Radiation Detection Company
Last Updated: March 17, 2026
Healthcare workers in imaging and interventional procedures face a daily tradeoff: managing physical strain from protective equipment while minimizing long-term radiation exposure. Understanding how radiation dose accumulates and how better awareness improves radiation safety can help workers reduce lifetime radiation risks while maintaining clinical efficiency.
In a conversation with Stephen Sabo, Healthcare Business Partner at Radiation Detection Company, and Chris Passmore, President of Radiation Detection Company, we explore a reality many imaging professionals face every day: balancing the physical strain of protective equipment with the long-term risks of radiation exposure.
Radiation exposure is a normal part of modern healthcare. Imaging technologists, interventional radiology teams, and cath lab staff rely on radiation to diagnose and treat patients every day.
But the radiation risks for healthcare workers are often invisible.
Unlike musculoskeletal pain from wearing heavy protective equipment, radiation exposure cannot be felt in the moment. The health impact comes from cumulative radiation dose over time, sometimes taking decades to appear.
In busy clinical environments where staffing shortages, long procedures, and fatigue are common, small decisions made for short-term comfort can quietly increase long-term radiation exposure.
Understanding this balance is essential for building a stronger culture of radiation safety and compliance.
Key Takeaways
- Radiation risks in healthcare settings often come from cumulative radiation dose over a career, not a single exposure event
- Physical strain from lead aprons and long procedures can influence radiation safety behaviors
- Radiation exposure is invisible, making awareness and monitoring essential for prevention
- Faster access to exposure data allows workers to adjust behavior and reduce dose earlier
The Physical Toll of Radiation Protection
For imaging professionals, radiation safety protocols often require wearing heavy lead aprons for extended periods.
Long procedures sometimes last several hours, and personal protective equipment (PPE) can put significant stress on the body.
Stephen Sabo, RT, (R), MBA, describes the physical realities many healthcare workers face:
“The physical toll is very real. The long procedures with a lot of standing, little movement lead to poor posture and then compensation, which can lead to eventual injury.”
In many hospitals, workers also face additional pressures:
- Staffing shortages
- Higher procedure volume
- Extended shifts
- Increased call coverage
Over time, the combination of heavy PPE and physical fatigue can create a difficult balancing act between comfort and protection.
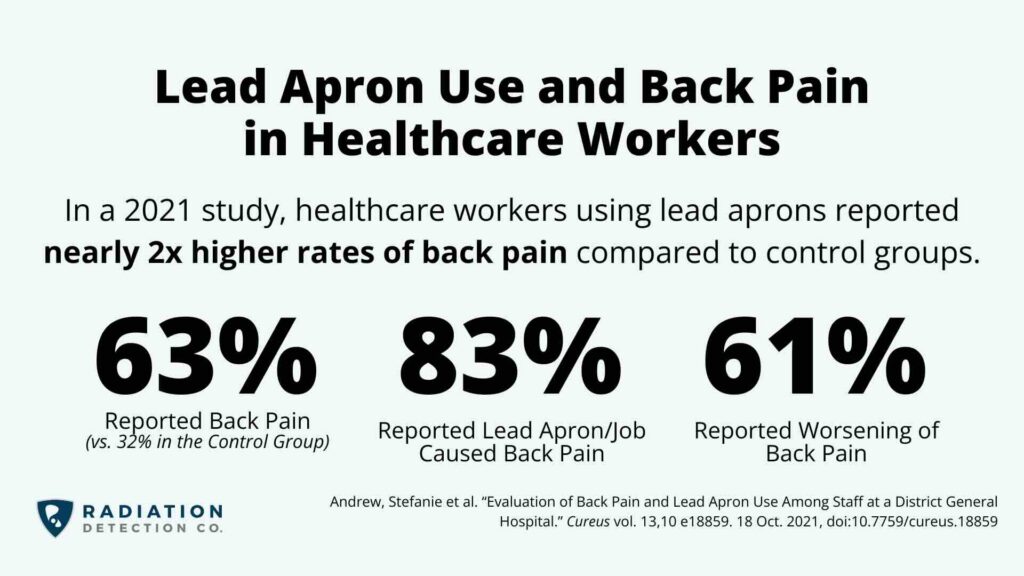
Chris Passmore, CHP, explains that musculoskeletal issues are common:
“A lot of cardiologists have a lot of back issues from wearing the lead apron for extended periods of time.”
For some workers, this leads to small adjustments that may reduce physical discomfort – and potentially increase radiation exposure.
Watch the Video: The Hidden Tradeoff in Imaging
The Invisible Nature of Radiation Risk
One of the biggest challenges in radiation safety is that exposure has no immediate sensory signal.
As Chris Passmore explains:
“It’s something you can’t feel, taste – you just have to be aware that it’s there.”
This makes radiation safety fundamentally different from other workplace hazards: when a worker lifts incorrectly, they feel pain immediately.
However, when radiation exposure occurs, the effects may take 10-20 years to appear. This delay creates an invisible risk that can easily fade into the background of busy workflows.
The Hidden Danger of Cumulative Radiation Dose
Radiation safety programs are built around a key scientific principle: cumulative exposure matters.
Even when each individual radiation dose appears small, the long-term effect of repeated exposure can increase cancer risk.
Chris explains that a widely followed principle, known as the linear no-threshold model (LNT), assumes that every exposure increases lifetime risk. With this philosophy in mind, radiation safety programs focus on reducing dose wherever possible.
“Every millirem of dose can increase your risk of getting cancer later in life. The philosophy is to try to keep that dose as low as possible.”
Over the course of a career, workers may accumulate exposure through:
- Thousands of imaging procedures
- Long fluoroscopy cases
- Improperly fitted shielding
- Inconsistent PPE usage
Understanding how radiation dose accumulates helps workers make better safety decisions.
Real-World Consequences of Occupational Radiation Exposure
Radiation safety has real human consequences.
Steve Sabo shares a powerful example from his experience working in hospital systems:
Two of the four founders of the cardiovascular program in Steve's old hospital system both died of pancreatic cancer because they wore thin aprons; they didn’t want to have problems later in life due to wearing a heavy apron all the time.
Radiology technologists and cardiologists face an increased risk of cancer related to occupational radiation exposure.
For Steve, this reality goes beyond risk – it’s personal. He lost a close friend and coworker to the same form of leukemia that he himself was diagnosed with just a few years later:
“As a leukemia survivor due to high radiation exposure, this conversation matters greatly to me. This is the reason I joined RDC.”
Chris notes that there are quite a few cancers associated with radiation exposure. The United States Nuclear Regulatory Commission (NRC) specifically acknowledges that leukemia, breast, bladder, colon, liver, lung, esophagus, ovarian, multiple myeloma, and stomach cancers are associated with high dose exposure.

These experiences reinforce a critical lesson: radiation safety programs exist to protect people. Regulatory compliance is important because it keeps workers, patients, and communities safe and healthy.
Steve recalls how the culture around radiation safety has shifted:
“In the late 80s and 90s, we were told to utilize high radiation doses to maximize the image quality of a CAT scanner. Now there's been a shift in radiation awareness, and over the last 20 years, technologies have come out to limit dose.”
However, Steve points out that increasing workloads and staffing shortages can make maintaining strict radiation safety practices more challenging:
“With the current staffing shortage, the technologists and physicians are still working long hours, taking call, the long cases, and being exposed to enough radiation where they need to take as many precautions as possible.”
How Better Awareness Improves Radiation Safety
One of the most effective ways to reduce occupational radiation exposure is to improve awareness of radiation dose; when workers can see how their behavior affects exposure, they can adjust techniques and reduce risk.
MyRadCare Insights™ automatically identifies risks and statistical outliers for better visibility, faster decision-making, and lower compliance risk.

Chris Passmore explains the value of timely dose feedback:
“The data is really important for the worker, because if they can correlate what they were doing at the time and how they were doing it, then they can make changes to their approach and reduce their dose.”
Data-driven radiation safety helps workers:
- Understand how positioning affects exposure
- Adjust shielding practices
- Improve procedural techniques
- Identify equipment or workflow issues
Chris notes that even small improvements repeated over time can dramatically reduce lifetime radiation dose:
"Without having a rad safety person being the ‘rad safety police,’ saying, ‘Back away now!’ or ‘Hey, you're doing that wrong.’ – they can self-correct in that scenario.”
Why Faster Dose Feedback Matters
Traditional dosimetry programs can be highly effective in environments where radiation exposure risk is relatively low and work patterns are consistent. However, in higher-exposure settings (such as interventional radiology, cardiology labs, or other high-volume imaging environments), more immediate visibility into dose can make a meaningful difference.
With digital dosimetry, workers have more immediate access to their exposure data. NetDose™ digital dosimeter can provide down to hourly readings.
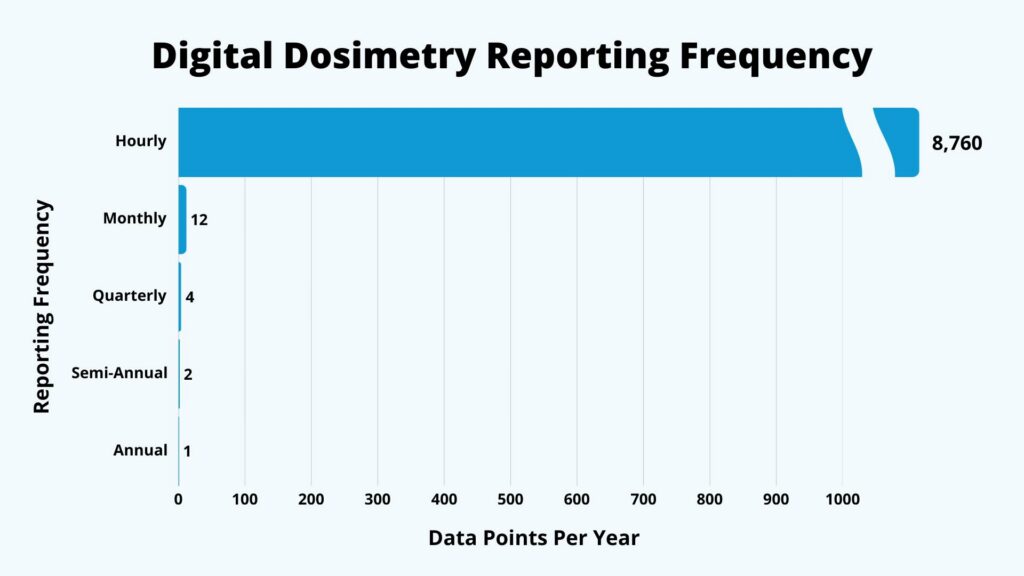
Chris Passmore explains the challenge:
“In really good performing laboratories, it'll probably take you 5 days to ship [dosimeter badges] to them after the wear period, and then about 5 days to process [them]. So, you're probably looking at a 10-day lag of data that you just don't know what's going on in that month prior.”
In some programs, results may take 30 days or longer. This delay can make it difficult for workers to identify what caused elevated exposure, and to course correct.
More immediate dose awareness allows workers to:
- Correct behaviors quickly
- Improve procedural technique
- Reduce repeated exposure events
Over time, these adjustments support a stronger culture of radiation safety and compliance.
Practical Ways Healthcare Workers Can Reduce Radiation Dose
Even in high-volume imaging environments, there are practical ways to reduce radiation risks.
ALARA, the core principle of radiation safety, calls for keeping radiation exposure as far below regulatory limits as practical by managing time, distance, and shielding as outlined below.
- Time: Limit time spent near radiation sources whenever possible.
- Distance: Maintain distance from the radiation source during procedures.
- Shielding: Use protective equipment and shielding correctly.
Stephen Sabo emphasizes the importance of staying mindful during procedures:
“No matter how tired you are, take precautions. Keep your distance from the radiation source, keep your shielding on. Unfortunately, dose is cumulative, so you want to take all the precautions you can, so you don't end up in a similar situation that I was in."
Chris acknowledges that if workers can quickly correct their behavior or technique, or realize that they need to get out of that radiation field and back away to reduce dose, those little incremental changes over time will make a big difference.
Building a Stronger Radiation Safety Culture
Improving radiation safety requires a culture built on awareness, education, reliable monitoring, and commitment.
Organizations that prioritize radiation safety often implement structured monitoring programs that combine accurate dosimetry data with modern management tools.
To learn more about how monitoring programs work, explore these resources:
- Ultimate Radiation Badge Guide
- Complete Dosimetry Program Management Guide
- Guide to Radiation Dosimeter Types: TLD, OSL & Digital Technology Comparison
These guides explain how organizations track radiation dose and maintain regulatory compliance.
How Healthcare Teams Can Reduce Long-Term Radiation Risk
Managing radiation risk and compliance requirements requires actively considering and protecting the people who care for patients every day.
In imaging environments, the pressures are real: long procedures, heavy protective equipment, and demanding workflows. Teams have to work to actively prioritize radiation safety – because lack of awareness doesn’t prevent radiation risk from building quietly over time.
Small decisions made in the moment to keep dose as low as reasonably achievable (ALARA), including increasing distance, using shielding, and limiting exposure time can shape a worker’s cumulative exposure across an entire career.
By improving awareness, providing clearer exposure insights, and reinforcing strong safety practices, healthcare organizations can help workers make better decisions in real time.
The goal is to give healthcare professionals the visibility and tools they need to reduce lifetime radiation dose while continuing to deliver exceptional patient care. When radiation safety becomes part of the organizational culture, it reduces the administrative burden – and manages risk.
Protect Your Workforce with Better Radiation Monitoring
Radiation Detection Company has supported occupational monitoring programs for more than 75 years.
If your organization wants to strengthen its radiation safety program, our team can help.
Contact our radiation safety experts now →
Frequently Asked Questions
What are the main radiation risks for healthcare workers?
Healthcare workers may experience increased cancer risk from long-term cumulative radiation exposure. Repeated exposure over many years, even at low doses, can increase the likelihood of certain cancers, particularly among workers performing high-volume imaging procedures.
How does radiation dose accumulate over time?
Radiation dose accumulates through repeated exposure events. Even small doses received during individual procedures can add up over a career, which is why monitoring and dose tracking are essential parts of radiation safety programs.
Why is radiation exposure difficult to detect?
Radiation exposure has no immediate physical sensation. Workers cannot see, feel, or smell radiation, which makes monitoring and safety protocols critical for maintaining safe working conditions.
What helps reduce occupational radiation exposure?
Three core radiation safety principles help reduce dose:
- Limiting time near radiation sources
- Increasing distance from radiation sources
- Using shielding such as lead aprons and barriers
Together, these practices significantly reduce exposure risk.
How do radiation monitoring programs improve safety?
Dosimetry programs track individual radiation exposure over time. This data allows organizations to identify trends, correct unsafe practices, and ensure workers remain within regulatory limits.