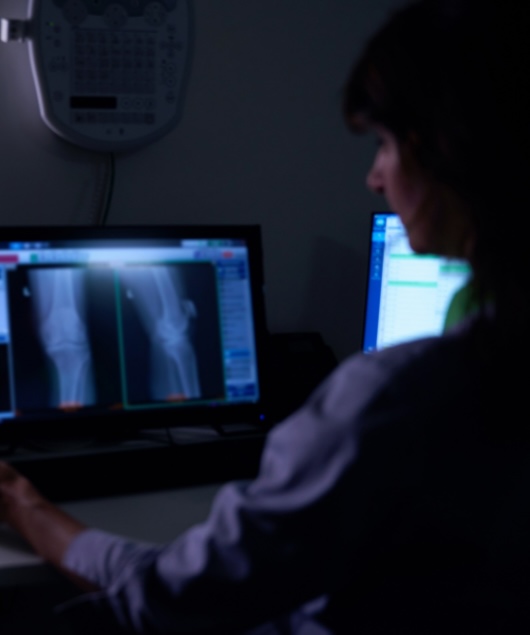
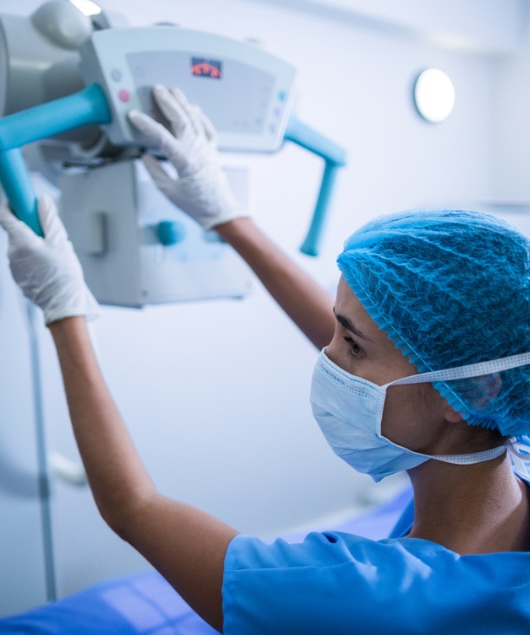
What Hospitals Should Be Asking About Their Dosimetry Service (But Usually Don’t)
Reviewed by
Chris Passmore, CHP
President, Radiation Detection Company
Last Updated: April 8, 2026
An inside look at how Radiation Detection Company answers the toughest questions about dosimeter badges, reporting accuracy, and compliance – so your program doesn’t fall short when it matters most.
The most important dosimetry service questions often go unasked, and most providers don’t make it easy to get answers.
At Radiation Detection Company (RDC), we believe transparency is part of the service itself. That means being willing to answer the hard questions – publicly, and clearly.
In a recent walk-and-talk at our headquarters, RDC President Chris Passmore, CHP, and Senior Vice President of Operations & Technical Services Mirela Kirr addressed six of the most important questions hospitals should be asking about their dosimeter badges, reporting timelines, and compliance support.
Unlike many providers, RDC is led by technical experts – health physicists responsible for overseeing operations, technology, and strategy – bringing a level of depth and accountability that’s uncommon in the industry.
Watch the Full Q&A Walkthrough
This post breaks down those answers – and more importantly, why they matter to your program.
Key Takeaways
- Turnaround time directly impacts compliance, investigations, and operational decisions
- Lost or damaged badges shouldn’t create administrative or regulatory risk
- Lower limit of detection (LLD) determines how meaningful your dose data actually is
- Many dosimetry services include hidden costs or gaps in support
- The OSL vs. TLD debate is often misunderstood and oversimplified
- The right provider reduces the burden on Radiation Safety Officers (RSOs) instead of adding to it
1. What is your typical turnaround time from badge receipt to dose report delivery?
Turnaround time is rarely the headline metric when organizations evaluate a dosimetry service, but it should be. At RDC, turnaround time is clearly defined.
Our turnaround time is 6 days from the receipt of the dosimeters.
Delayed reporting creates a dangerous gap between exposure and awareness; depending on your provider, you might have to wait up to 20 days for your dose reports. In high-risk environments, that delay can extend into the next monitoring period.
The time between badge receipt and report delivery directly affects how quickly an organization can respond to potential exposure events, complete internal reviews, and maintain audit-ready documentation. Delays create inconvenience, administrative burden, and risk.

At RDC, we treat turnaround time as a core performance indicator. The goal is to deliver accurate dose reports as quickly as possible after badge receipt, ensuring that data remains actionable when it matters most. If your reports are consistently delayed, you’re operating without awareness.
Timeliness is a safety and compliance requirement – it’s a risk control mechanism.
For a deeper look at how reporting fits into a complete program, see the Complete Dosimetry Program Management Guide: Setup, Compliance & Cost Optimization.
2. How do you handle lost, damaged, or late badges?
Every dosimetry program encounters exceptions. Badges are lost, returned late, or damaged in the field. The difference is how those exceptions are managed.
A well-structured dosimetry service should guide organizations through these situations with clarity and consistency. That includes establishing documented processes for dose estimation, maintaining compliance records, and resolving issues quickly without creating additional administrative burden.
Where many providers fall short is in turning these exceptions into friction – either through unclear policies, slow response times, or unexpected costs.
At RDC, we proactively identify missing or late badges in the same reporting cycle so the client can take the right action.
The focus is on minimizing disruption. When something goes wrong, the process should still feel controlled, compliant, and predictable. Even more importantly, RDC is building systems that go beyond tracking into prediction and resolution.
MyRadCare Insights™ is a powerful radiation safety analytics platform designed for healthcare systems that demand better visibility, faster decision-making, and lower compliance risk.

With MyRadCare Insights™, RSOs identify patterns among workers with behavioral tracking to help communicate which dosimeters are late before they are truly late. The platform can also help estimate the dose and update records for lost or damaged dosimeter badges.
Move from data to decision faster with MyRadCare Insights™ →
3. What’s the lower limit of detection (LLD) for each dosimeter badge type?
The lower limit of detection (LLD) is one of the most technical aspects of a dosimetry program – and also one of the most misunderstood.
At its core, LLD reflects how well a dosimeter can report dose accurately over time. A key nuance many providers overlook is that LLD is not a static number – it changes based on wear period/frequency.
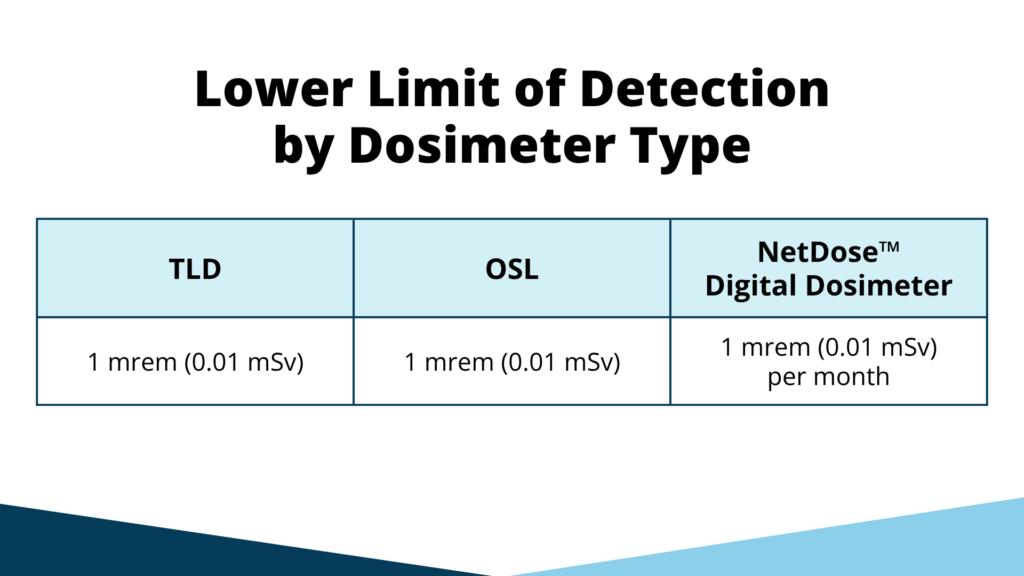

In environments where exposure is low or variable, this becomes critically important. A reading of “zero” doesn’t always mean no exposure occurred – it may simply fall below the detection threshold.
RDC’s technology is designed to maintain sensitivity over time: our dosimeters can see well below 1 millirem, even over a full month.
Different badge technologies (such as OSL, TLD, and digital systems) offer different levels of sensitivity and performance. Understanding these differences is essential if you want your data to reflect reality, not just thresholds.
For a deeper understanding, check out our Guide to Radiation Dosimeter Types: TLD, OSL & Digital Technology Comparison.
The takeaway is simple: if you don’t understand your LLD, you don’t fully understand your data.
4. What does dosimetry service include at Radiation Detection Company? Any hidden fees to watch out for?
This is one of the most important questions organizations can ask, and one of the least transparently answered in the industry.
On the surface, most dosimetry services appear similar. Badges are issued, processed, and reports are delivered. But the details of what’s included (and what’s not) can vary significantly.
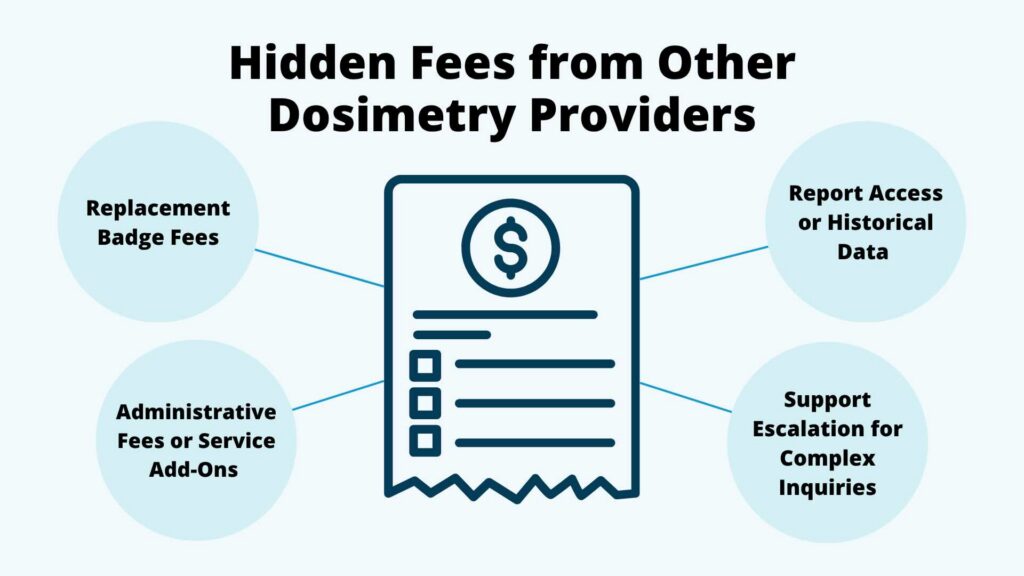
At RDC, our dosimetry service pricing is intentionally simple and transparent. We have extremely few fees: we don’t charge for participant setup, reporting, or investigations.
This stands in contrast to common industry practices that introduce hidden costs over time. Chris highlights one of the most surprising examples:
“The craziest charge I’ve seen is charging to set up a new participant.”
For a full breakdown of common hidden fees and what to watch out for, check out our blog: How Dosimetry Badge Pricing Works.
A comprehensive service should extend beyond basic processing to include reporting access, data management, customer support, and compliance guidance as part of a unified offering – not fragmented add-ons.
If you don’t fully understand your dosimetry service agreement, you’re likely paying for gaps you didn’t know existed.
These hidden costs impact budgets and create administrative burden for RSOs who must audit invoices line-by-line. RDC’s approach removes that friction, so teams can focus on safety – not billing validation.
For accurate pricing based on your workforce and monitoring needs, call 800.250.3314, use our pricing calculator, or complete our contact form.
5. What’s the most common misconception people have about OSL vs. TLD?
The most common misconception around OSL and TLD technologies is that one is universally better than the other. In reality, both OSL and TLD are highly capable – and the right choice depends on how each performs within your specific environment and workflow.
At Radiation Detection Company, we offer both OSL and TLD dosimeter badges because our goal is to help you choose what actually fits your program.
One area where confusion often shows up is around detection performance and long-term reliability.
“There’s a misconception that only certain OSL dosimeters can achieve low detection limits. We’ve shown ours can outperform many others.”
– Chris Passmore, CHP
Detection sensitivity is only part of the picture. Long-term performance matters just as much – especially in healthcare environments where badge programs scale across large teams.
Our dosimeters have less than 3-4% fade per year – fade is the loss of signal over time in the dosimeter. Lower fade enables longer wear periods, which reduces administrative workload for hospitals.
That low fade rate has a direct operational impact. It enables longer wear periods without sacrificing accuracy, which reduces how often badges need to be exchanged. For hospitals managing hundreds or thousands of badges, that translates into less administrative burden, fewer exchanges, and a more efficient program for RSOs.
Ultimately, the goal isn’t to choose the “newer” or “better” technology – it’s to choose the one that delivers reliable data, operational efficiency, and compliance confidence in your environment.
Both OSL and TLD technologies are widely used, well understood, and effective in the right environments. RDC’s systems are designed for both accuracy and long-term durability.

We broke down the technical differences further in our Guide to Radiation Dosimeter Types: TLD, OSL & Digital Technology Comparison.
Ultimately, the decision should be based on program needs, not assumptions about technology. Factors like exposure variability, workflow complexity, and reporting expectations all influence which option is most appropriate.
Need more support in determining which dosimeter badge will work for your organization? We’re here to help. Call 800.250.3314 to speak directly with a dosimetry specialist or complete our contact form.
6. How do you support organizations with compliance needs? How do you simplify the day-to-day work of Radiation Safety Officers (RSOs)?
At Radiation Detection Company, we believe a dosimetry provider should go beyond the bare minimum expectation of delivering timely reports to actively reduce the complexity of managing a radiation safety program.
For RSOs, the day-to-day reality often involves tracking badge usage, resolving exceptions, preparing for audits, and ensuring documentation is complete and accessible. Without the right support, these responsibilities quickly become overwhelming.
At RDC, the approach is to simplify these workflows through centralized systems, responsive support, and proactive guidance. Our customer platform, MyRadCare™, provides a single point of access for reporting and data management.

We also provide expert support to ensure our customers’ compliance questions are addressed quickly and accurately. In this way, RDC acts as an extension of the RSO’s technical knowledge.
Chris shared one example involving a contaminated dosimeter with unusually high readings – an event that initially created significant concern for the client.
Rather than simply reporting the result, RDC analyzed the data pattern, understood how the dosimeter responded, and worked to reconstruct what actually happened.
As Mirela explains: “We were able to design the exact scenario that happened … based on what we knew about the radiation field and how the dosimeter performed.”
In this case, the team determined that a strontium source had been placed directly on the dosimeter – something that wouldn’t have been obvious from the raw data alone.
Chris shared how the real validation came next: “We got the exact same result. We told them exactly how long to put the source in contact with the dosimeter to replicate the exposure – we were within a couple seconds.”
That level of precision allowed the client to confidently determine what occurred and whether the exposure was occupational or incidental, turning a stressful, ambiguous situation into a clear, defensible outcome.
This is where dosimetry moves beyond reporting and becomes an active investigation and compliance tool.
Our dosimeters tell a story about how exposure occurred.
For RSOs – especially in smaller hospitals – this kind of partnership is critical. Every organization deserves a program that feels manageable and proactive – that’s what’s best for the health of each employee, and the health of your organization.
For larger organizations with high-exposure environments like fluoroscopy and cath labs, that means moving beyond reactive reporting. With MyRadCare Insights™, teams gain proactive, real-time, exception-based visibility that enables faster decisions and tighter control over compliance risk.
“RDC makes it easy for organizations to protect employees working with radioactive materials and radiation-emitting equipment. We listen to our customers and actively invest in our technology and IT infrastructure to ensure continuous service and exceptional customer care.”
– Chris Passmore, CHP
Bonus: How do you manage the transition if we switch dosimetry providers?
Switching dosimetry providers is often perceived as disruptive, but with the right process, it doesn’t have to be.
At Radiation Detection Company, we’ve built SwitchAssist™ specifically to remove the friction from transitioning programs. Instead of placing the burden on your team, we guide the process end-to-end to ensure continuity, compliance, and minimal operational impact.
That includes coordinating badge changes, aligning wear periods, transferring historical data where needed, reminding you of typical contract cancellation terms and vendor notifications, arranging ship date timing, and ensuring your reporting remains consistent and audit-ready throughout the transition.
The goal is simple: no gaps in monitoring, no confusion for staff, and no added administrative burden for RSOs.
Most organizations delay switching because they assume it will be complex. In reality, with a structured onboarding process, the transition can be smooth and often results in immediate improvements in reporting, visibility, and support.
At RDC, account setup typically takes 1-3 days, depending on organization size and account complexity – we can set up your account and get ship dosimeters to you before most providers can even enter your account information.
See what you could save in time, administrative burden, and costs with our pricing calculator, or complete our contact form for a custom quote.
Why These Questions Matter More Than You Think
Most organizations evaluate dosimetry providers based on what’s easiest to compare: dosimeter price, contract terms, or familiarity.
The real differences emerge over time, in the details that aren’t always visible upfront:
- How quickly reports are delivered
- How exceptions are handled
- How clearly data can be interpreted
- How much time your team spends managing the program
We’re answering these questions publicly because transparency reflects our company values. At RDC, that means Integrity First, a Relentless Commitment to Quality, and a focus on Human Connection in everything we do.
And if you watch through to the end, you’ll see our final value in action too: Serious Work, Fun Workplace.
Better Questions Lead to Better Programs
A strong dosimetry program starts with asking the right questions. If your current provider isn’t proactively addressing these areas, it may be worth taking a closer look at what’s happening behind the scenes.
In radiation safety, gaps are rarely obvious – until they become problems.
At Radiation Detection Company, we believe organizations should have complete confidence in their dosimetry service, their data, and their defensible regulatory adherence.
Ready to Evaluate Your Dosimetry Program?
If you’re unsure how your current program stacks up, we can help.
Call 800.250.3314 to speak with a dosimetry specialist →
Complete our contact form to talk to a sales representative →
Frequently Asked Questions
What is included in a dosimetry service?
A dosimetry service typically includes badge processing, dose analysis, reporting, and compliance support. However, the scope can vary significantly, so it’s important to understand what is included and what may come at an additional cost.
How accurate are dosimeter badges?
Accuracy depends on the badge type, calibration, and environmental conditions. Understanding the lower limit of detection (LLD) is essential for interpreting results correctly.
It’s also important to consider fade as a function of time. As a dosimeter is worn, signal loss can occur, which impacts how accurately dose is measured over the full wear period. Technologies with low fade maintain accuracy over longer durations, while higher fade can reduce confidence in results – especially for extended wear periods.
Together, LLD and fade determine how well a dosimeter captures true dose over time, not just at a single point of measurement.
What happens if a badge is lost?
A compliant program should include a clear process for estimating dose, documenting the incident, and maintaining audit readiness without unnecessary administrative burden.
Is OSL better than TLD?
Not universally. While older TLD-100 technology was less comparable, advancements in detector materials have significantly narrowed the gap. Modern LiF:Mg,Cu,P TLD and BeO OSL technologies are both highly effective and capable of delivering accurate results.
At RDC, we utilize lithium fluoride, copper-doped TLD (LiF:Mg,Cu,P) due to its strong tissue equivalency, which supports more accurate dose measurement in real-world conditions.
Ultimately, the right choice depends on your specific environment, workflow, and data requirements – not the technology alone.